MAY 7, 2020

Couples wearing face masks amid concerns over the COVID-19 novel coronavirus walks through a market in Seoul on April 22, 2020.
The tulips were blooming in Seoul and Dr. Jerome Kim was strolling in his government-issued KF-94 mask with his wife when he got a text message alerting him to a confirmed coronavirus infection in his neighborhood.
It was early April and South Korea made headlines around the world for effectively containing the first major Covid-19 outbreak outside of China by testing broadly throughout the population and tracing contacts of infected individuals. But now students were returning from abroad and bringing the virus with them.
Kim, who serves as the Director-General of the International Vaccine Institute, clicked on the alert on his phone and it directed him to the municipal site, which detailed the infected individual’s whereabouts over the past several days.
The individual, who was anonymous, had visited a local supermarket on a recent Saturday between 10 a.m. and 10:15 a.m. to buy chilies, which was confirmed with CCTV footage and credit card transaction data, Kim recalled.
Text alerts
“My wife and I kind of looked at each other and said, ‘well, we were there … but on Sunday,'” he said with a laugh. “It’s one of those balances of privacy versus public good, but it’s a decision governments need to make, and in South Korea I think it’s made all the difference.”
That alert was one of dozens, if not hundreds, that millions of South Koreans have received since the coronavirus arrived in the country on Jan. 20, Kim said. He added that such sharing of information, despite its data privacy implications, has helped to keep the infection rate down even as businesses reopen.
While Hong Kong and South Korea have largely succeeded in containing the epidemics in their borders without enforcing the most restrictive policy measures, Singapore, Japan and China have all struggled to do the same. The varying results of efforts across Asia to contain the virus and reopen businesses has taught researchers and public health specialists about the nature of the virus and given policymakers proven methods to fight it.
“This virus likes to find opportunities to spread and if these lockdown measures are lifted too quickly, the virus can take off,” Dr. Maria Van Kerkhove, the World Health Organization’s lead scientist on Covid-19, said Wednesday. “The only way to control and suppress this virus, this Covid-19, is to actually find [cases], quarantine those contacts, isolate the cases and it will be brought under control.”
From data sharing and border closures to targeted contact tracing, some policies have proven more effective than others. Countries that were hit later by the virus are at an earlier stage in cycle of the outbreak and have a distinct advantage: insight into what succeeded and failed in other countries in Asia. However, public health specialists who spoke with CNBC said they’re not confident U.S. officials are taking note of what’s working and what has failed overseas. They predict the virus will likely bounce back in the U.S. as it has in Singapore and Japan.
Singapore
“This is a tough, tough virus,” said Dr. Dale Fisher, the chair of infection control at the National University Hospital and the National University of Singapore. “All it takes is one infected person and it spreads like wildfire.”
Singapore appeared to have their outbreak under control in February. After reporting its first confirmed case on Jan. 23, businesses remained open for months as health officials developed a plan to prevent community-wide transmission by tracing contacts of infected individuals and isolating them. The wealthy city-state shut its borders to travelers from at-risk countries to avoid importing the disease on March 23, after confirming its first two Covid-19 deaths, but still didn’t lock down businesses.

A man leans on his cane outside the closed Jamaica flower market, in Mexico City, Mexico, on May 7. While some flower vendors with shops still open outside the market, the large, wholesale flower market temporarily closed for one week starting Thursday, ahead of Mother’s Day in an effort by the city to keep the usual holiday crowds away.
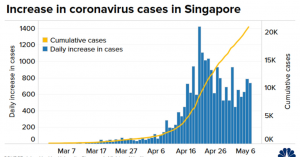
By March 31, the country had reported just 879 confirmed cases and three deaths on the island nation, according to data collected by the World Health Organization. The virus started picking up in speed in Singapore in early April. By April 10, the number of confirmed infections more than doubled to 1,910 and it hasn’t slowed since.
However, Singapore’s response overlooked a crucial segment of the population, Fisher said: the hundreds of thousands of foreign workers upon whom the island nation depends for low-wage labor. The virus began to spread throughout the overcrowded and unsanitary dormitories that house these workers, said Fisher, who also serves as chair of the WHO’s Global Outbreak Alert and Response Network. It has since erupted into Southeast Asia’s largest outbreak.
The country reported 632 new cases on May 6, bringing total infections to 19,410, according to the WHO’s data.
Vulnerable population
The government, assuming the virus has already swept across much of the migrant population, has quarantined tens of thousands of workers in massive factories that have been converted into isolation wards, Fisher said. He added that the daily new case count remains impressively under 30 or so in the general population, but hundreds of new cases are reported in the wards everyday. Fisher said Singapore’s hospitals are now mostly full and officials are scrambling to boost capacity.
“You cannot overestimate this virus’ ability to find vulnerabilities in society and these are often vulnerabilities that amplify socioeconomic differences,” Fisher said. “Every country that’s under lockdown I think has a crux in the outbreak it wishes it could go back to and I guess at the moment, Singapore is wishing it could go back to the early days in those dormitories.”
Fisher said he hopes U.S. policymakers have taken note of the situation in Singapore. However, as officials in places like New York, New Jersey and Detroit wrestle with the United States’ largest epidemics, the concentration of infections appears to have shifted to vulnerable people in the U.S.
Infections are accelerating rapidly among prisoners in the U.S., The Marshall Project reports, with more than 14,000 confirmed cases so far as of April 29.
The Smithfield Foods pork factory in Sioux Falls became the biggest coronavirus hot spot in the country and was forced to close last month after confirming 238 active cases as of April 12, accounting for 55% of the state’s total at the time, South Dakota Governor Kristi Noem said. Last week, the CDC said about 3% of workers in over 100 meat processing plants have tested positive for the coronavirus. As the virus circulates among prisoners and low-wage factory workers, such groups could become vehicles of transmission even as the outbreak is stamped out elsewhere.
‘Threat of war’
South Korea is one of the few countries that has prevented a sustained Covid-19 epidemic without steamrolling its economy. Instead of quarantining entire cities like China and shuttering businesses and factories like Europe and the U.S., it implemented the world’s biggest testing and tracing program.
Between Jan. 19 and Feb. 18, South Korea confirmed a total of 31 cases, most of which were directly linked to travel to hot spots in China, according to data compiled by the WHO. In the weeks that followed, the virus spread to multiple cities across the country. New cases peaked on Feb. 29, when the country reported 813 new cases, bringing the total to 3,150, according to WHO data.
Total cases more than doubled by March 10, but Korean health officials rolled out an aggressive testing regime that processed tests for more than 259,000 people and confirmed more than 8,000 infections by mid-March, according to the Korean CDC. The U.S., by comparison, had tested roughly 22,000 people by then, according to the U.S. CDC at the time.
South Korea set up hundreds of walk-in and drive-thru testing centers, traced the origin of local outbreaks and isolated people who might have come in contact with the virus. The rate of infection plateaued at around 100 new cases per day for much of March and early April.
Flattened the curve
Their success was punctuated on April 15 when the country held its parliamentary election, which garnered the highest turnout of a national election since 1992. In the days that followed, daily new cases dropped to single digits. On May 6, the country reported just two new cases.
“South Korea successfully flattened the curve on Covid-19 in 20 days without enforcing extreme draconian measures that restrict freedom and movement of people,” reads a study published by the Korean government last month called “Flattening the curve on Covid-19: the Korean experience.” The government issued it as a policy guide to maneuvering the pandemic.
Since the South Korean government never enforced a full lockdown, voluntary compliance has been key, Kim said. The government has encouraged employers to let nonessential personnel work from home, Kim said, and distributes free equipment like masks to every household that requests it. Government messaging has been clear, consistent and mostly communicated by health officials rather than politicians, he said, which was key to mobilizing the public.
“Koreans have lived under the threat of war since the Korean War and this is like a war,” Kim said. “We’re going to do what we need to do to get through it. This is just part of living here, so people got used to it. The government pulled people together.”
Watching Americans protest social distancing requirements outside state capitals across the U.S., Kim said he wasn’t confident U.S. citizens could be as disciplined as South Korea. Mixed messaging from the White House and state leaders about economic reopening has not helped the public, he said.
Data sharing
After the MERS outbreak in 2015, Korean lawmakers passed the Infectious Disease Control and Prevention Act, which established not only the authority, but also the duty of the Ministry of Health to collect and share location-tracking data of every infected individual if an outbreak rises to the established level of severity.
“I think countries need to decide for themselves, but in South Korea we had that debate in the intervening period between 2015 and 2020,” Kim said. “That’s the time to have that discussion, when you’re calm and when you have the lessons of a furious outbreak behind you.”
That level of sharing by the government stands in stark contrast to the U.S., where some municipal, county and state coordination is often challenged. Some states only break out coronavirus cases at the county level and even then the data is lagging by several days and paper work is processed between hospitals and authorities.
In a country as vast as the U.S., tech-driven contact tracing could be key to monitoring the virus, public health officials say. Apple and Google announced a partnership in California last month to develop tools to conduct just this kind of tracing, though its unclear when and if it will be adopted generally across the country.
Hong Kong
Hong Kong saw several localized outbreaks across the city, many of which were imported from mainland China in February and March, Dr. Keiji Fukuda of the University of Hong Kong said. He added that the city managed to contain the outbreaks with rigorous testing and tracing as well as by implementing some limited social distancing measures.
By March 15, the city had reported just 149 cases.
However, daily new cases bounced back in late March and early April as travelers, and many students who had been studying abroad returned to Hong Kong, said Fukuda, who previously served as assistant director-general of health security at the World Health Organization. Of Hong Kong’s 1,045 total cases as of May 7, 619 were imported, according to Hong Kong authorities. Fukuda added that understanding the dynamics of the virus like that is key to enacting effective policy.
“If you have infections coming in from the outside, you want to be thinking about it one way,” Fukuda said, “and if they’re occurring inside inside the country, then you know it makes sense to be thinking about it in a different way.”
Hong Kong closed its international border to travelers from most countries on March 23. Those still allowed to enter, are compelled into a mandatory 14-day quarantine. Even as daily new cases have hit zero on some recent days, health officials remain watchful, said Dr. Ben Cowling, professor of infectious disease epidemiology at the University of Hong Kong.
“If those border restrictions were relaxed, that will be a big problem,” he said, adding that reopening the border selectively could be a point of international collaboration in the future.
Lifting lockdowns
Just as international travel has driven the outbreak in Hong Kong, domestic travel across the U.S. could spur transmission, Cowling said. North Carolina’s very first coronavirus case in early March was imported from Washington state, public officials said at the time. The patchwork policies of states lifting regulations will only encourage interstate transmission and exacerbate infection, he said.
“When I think about the U.S. coming out of lockdowns, I think transmission across the country will be a big threat and I don’t know how it could be dealt with,” Cowling said. “If places come out of lockdown and have a low level of cases, but then there’s people coming in from the cities in large numbers often, even if only a tiny fraction are infected, that can still be the seeding for local outbreaks to start again.”
The lack of federal leadership in lifting restrictions could create a situation in which states will need to lockdown again, said Yanzhong Huang, public health researcher at the Council on Foreign Relations. He added that as the population mixes, especially as people currently in states with heavy restrictions leave for more relaxed states, they could bring the virus with them, sparking local outbreaks in pockets outside of cities.
Outbreaks vary by state
“The spread of the virus has varied state to state, so the prevention measures adopted also vary state by state,” Huang said. “That means the plateau, the peak of the virus also varies state to state. It’s one of the biggest problems, how to deal with this variation in terms of the trajectory of the spread of the virus.”
The experience of Hong Kong and other cities and regions in China and Japan that have similarly seen an influx of imported cases raises important questions about travel amid the pandemic, said Olga Jonas, senior fellow at the Harvard School of Public Health and former World Bank economist.
She said she hopes there’s enough U.S. surveillance testing and tracing infrastructure in place by the summer so that people can travel. But she said unsuspecting travelers could be vehicles for the virus and if pockets of infection threaten to overwhelm society so that it has to shut down again, the economic consequences could be even more devastating.
“The big lesson is that while the coronavirus pandemic is not under control anywhere in the world, it’s a threat to everywhere else,” she said. “Any kind of travel is going to add to the risk of transmission.”
Courtesy/Source: CNBC