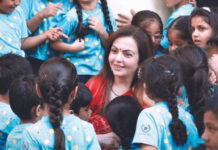MAY 4, 2020

Omandurar Medical College hospital pictured in Chennai, India, on May 3, 2020. – Arun SANKAR / AFP
Scientists have identified an antibody in a lab that they say can prevent the novel coronavirus from infecting cells. The team hopes the antibody could be used to create treatments for COVID-19, the disease caused by the virus.
Since the coronavirus began infecting people in the central Chinese city of Wuhan late last year, more than 3.5 million people have been diagnosed with COVID-19, over a million have recovered and almost 248,000 have died, according to Johns Hopkins University.
The team, whose research was published in the journal Nature Communications, have been exploring whether what are known as monoclonal antibodies could help patients with COVID-19. Currently there is no vaccine or specific treatment for the disease. Monoclonal antibodies are a type of protein created in a lab which can bind to a specific substance in the body. These types of antibodies mimic how the immune system responds to a threat, and are used to treat some forms of cancer.
An antibody named 47D11 was found to bind to the spike protein which the novel coronavirus, known as SARS-CoV-2, uses to enter the body, and block it in a way that neutralizes the pathogen.
To carry out their study, the researchers used mice whose biology was tweaked to create antibodies similar to those found in humans. They injected the animals with spike proteins that the viruses which cause SARS, MERS, and some types of common cold use to invade cells. These viruses are members of the large coronavirus family of pathogens which also includes SARS-CoV-2, the bug which causes COVID-19. The mice produced 51 antibodies capable of neutralizing the spike protein of the injected coronaviruses. This stage of the research was done before SARS-CoV-2 first came to the attention of health officials in late 2019.
The team later watched to see if the antibodies would neutralize SARS-CoV-2 and SARS-CoV in lab samples, and found 47D11 did.
Co-author Berend-Jan Bosch, associate professor of the Utrecht University Infection and Immunity programme, explained in a statement that the research builds on work his team had done previously on antibodies which can target SARS-CoV, the virus which causes SARS.
“Using this collection of SARS-CoV antibodies, we identified an antibody that also neutralizes infection of SARS-CoV-2 [the COVID-19 virus] in cultured cells. Such a neutralizing antibody has potential to alter the course of infection in the infected host, support virus clearance or protect an uninfected individual that is exposed to the virus.”
Co-author Frank Grosveld, Academy Professor of Cell Biology at the Erasmus Medical Center, Rotterdam, said: “This discovery provides a strong foundation for additional research to characterize this antibody and begin development as a potential COVID-19 treatment.”
Experts not involved in the research welcomed the findings, but also pointed out the study’s limitations.
Tony Carr, professor of molecular genetics in the Genome Damage and Stability Centre (GDSC) at the University of Sussex, said in a statement: “The block to infectivity is entirely based on cell culture work, but the previous literature supports the proposal that this reagent should be explored further as a potential treatment.”
Penny Ward, visiting professor in Pharmaceutical Medicine at King’s College London, said the antibody has the potential to be used to prevent and treat SARS-CoV-2 infection, “however without studying this in an animal model, it is not clear which of these approaches might be most efficient.”
The findings would have been more robust if the team were able to show the antibody could prevent and treat COVID19 in animals, she said.
“It is not possible to conclude that the product will be effective in vivo in humans,” said Ward.
Polly Roy, professor of virology at the London School of Hygiene and Tropical Medicine, said the data the team created is “very good,” and highlighted they are well-known for their work on coronaviruses.
Gary McLean, professor in Molecular Immunology at London Metropolitan University, said: “Because it is not done in people and the antibody is not even found in people as far as we know there are limitations. However it is a nicely done study that could provide a potential biotherapeutic that could be used to treat COVID-19.
The research complements separate projects looking at whether a century-old technique known as convalescent plasma therapy, where the blood from a person who has recovered from COVID-19 is inserted into a current patient in the hope it will help them beat the disease.
Professor Babak Javid, principal investigator at Tsinghua University School of Medicine, Beijing, and consultant in infectious diseases at Cambridge University Hospitals in the U.K., commented: “This is a very interesting study. One of the most widely touted experimental (though not yet proven) treatments for COVID is the use of convalescent plasma.”
He said: “However, use of convalescent plasma is difficult to scale and make widely available as a treatment and has some potential safety concerns since it is a blood product. Therefore there has been intense scientific interest in identifying individual antibodies that can also neutralize SARS-CoV2. This is because we are able to manufacture large quantities of individual antibodies (known as monoclonal antibodies or mAbs) at scale as a pharmaceutical treatment for COVID. Monoclonal antibodies also don’t have the safety concerns of administering blood products.”
Simon Clarke, associate professor in Cellular Microbiology at the University of Reading, U.K., said in a statement: “Antibodies like this can be made in the lab instead of purified from people’s blood and could conceivably be used as a treatment for disease, but this has not yet been demonstrated.
“While it’s an interesting development, injecting people with antibodies is not without risk and it would need to undergo proper clinical trials.”
Courtesy/Source: Newsweek