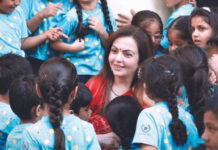DECEMBER 22, 2022

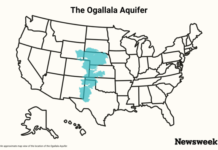
Dr. Anthony Fauci prepares to speak about COVID-19 at the White House in April 2020. (Alex Brandon / Associated Press)
Dr. Anthony Fauci, who turns 82 on Saturday, wants the record to reflect that he is not retiring. Really, he isn’t. It’s just that after 54 years as a government scientist and advisor to seven presidents, he is leaving the National Institutes of Health at the end of the year.
The nation’s top infectious disease doctor insists he still wants to write, make public appearances and continue to shape research on infectious diseases. So he will continue to be a presence in the lives of his many fans — and his equally zealous detractors.
As Fauci tells it in his distinctive Brooklyn accent, he drove onto the NIH campus in Bethesda, Md., in June 1968, a 27-year-old physician fresh out of residency training. He burrowed into the burgeoning field of immunology and was well situated to help identify the source of a mysterious illness afflicting gay men in the early 1980s.
Fauci went on to lead the federal government’s efforts to bring HIV/AIDS to heel after becoming director of the National Institute of Allergy and Infectious Diseases in 1984. In the decades that followed, he was key to shaping the U.S. response to the H1N1 flu pandemic, the Ebola outbreak and the Zika virus.
When a mysterious pneumonia-like illness was identified in Wuhan, China, in December 2019, Fauci was still at the helm of NIAID. His poker-faced visage loomed behind then-President Trump as the leader of the free world boldly predicted the virus would miraculously disappear.

President Trump speaks during a coronavirus task force news conference March 20, 2020, as Dr. Anthony Fauci, far right, looks on. (Al Drago / Bloomberg via Getty Images)
It didn’t, prompting Trump to call Fauci a “disaster” and helping spawn a legion of trolls whose violent threats against the doctor and his family soon necessitated an armed security detail. Trump even wished aloud that he could fire Fauci but ultimately decided that doing so would detonate a “bigger bomb” than keeping him on.
In addition to keeping him on as head of NIAID, President Biden made Fauci his chief medical advisor, a valediction to more than a half-century of public service. Fauci spoke with The Times about his career and the continued fight against infectious disease.
Your career has been bookended by the HIV/AIDS and COVID-19 pandemics. Both diseases are still with us, and are likely to remain so for some time. Do you find that discouraging?
Not at all. The work with HIV is historically transforming. When we first started caring for patients, we would give an infected patient a life expectancy of eight to 12 to 15 months. Almost all of my patients died.
Over a period of time, we discovered the virus and developed a diagnostic test. And over a few years, we developed a series of antiretroviral drugs, then we added the protease inhibitor. Today we can tell somebody who’s infected with HIV that if they get on therapy, they are going to live an essentially normal lifespan.
And now, we have drugs that can 99% prevent infection with HIV. It’s true we don’t have a vaccine yet for HIV/AIDS, but hopefully we’ll get it.
That’s the science thing that I’m responsible for. I’m not responsible for the implementation of healthcare systems that don’t get people into healthcare. I’m not responsible for the fact that there’s a lack of equity. What I have been responsible for is the science, and the science has been an overwhelming success story when it comes to therapy and prevention. So am I discouraged? No, I think it’s cause for celebration!
The public seems to expect quick, complete solutions. Do they fail to appreciate that science doesn’t quite work that way?
I think there is a lack of appreciation for that. With HIV it was a gradual process of going from a complete lack of interventions in the early 1980s, to fielding interventions that proved slightly effective in 1986-87, then progressively adding medications that were moderately effective, and now to having drug combinations that are universally and dramatically effective.
I think people think of science as something that you get up at bat and you hit a home run the first time around. It isn’t that way — it’s a gradual, iterative process that is cumulative, and that will ultimately get you to the endgame you want.
And when the progress of science takes an unexpected turn?
That’s another lesson learned. Science collects data, and you act on the data that you have at the time.
In January 2020, we were learning about aspects of the coronavirus, and we had to, by necessity, make recommendations, make guidelines. We had to publicly discuss our understandings of the virus.
But the outbreak was dynamic, and science is self-correcting. So what we knew in January was one thing. When we later learned that the virus is readily spread by aerosol, and that 50% to 60% of the spread was by people who didn’t even know they’re infected, we had to change our recommendations and guidelines.
People sometimes said, “You’re flip-flopping.” It has nothing to do with flip-flopping! It was a case of continuing to make decisions based on the latest and most accurate data you have. After all, the SARS-CoV-2 that we were dealing with in January 2020 was very different from the SARS-CoV-2 virus that we’re dealing with now.
If you stick with the science, you’re going to have to be prepared to change as the facts evolve.
You’ve had more experience communicating with the public than most scientists will ever have. What has that taught you?
That people don’t hear the caveats. They hear the positive aspects of what you say.
As we communicate what we know, the only thing we can do better is to continue to try to emphasize that we’re dealing with a moving target, and that what we’re telling you now is based on the data as we know it. However, this may change, and we may need to change.
Yet every time I’ve done that, the headline never includes the “however.” They never, ever include the caveat.
The science of immunology is enormously complex. Yet people without science background need to understand enough of it to make sense of your recommendations. How do you deal with that?
You have to take special care in articulating its complexity. And you just have to keep the “however” in the explanation.
I don’t blame the public. But it is truly complicated — the whole idea of antibody immunity that goes up and then goes down, and the T cells that persist but are tough to measure, though they’re probably the most important thing protecting you from severe disease. It’s so difficult to get that into a soundbite. You can’t report immunology in two sentences.
What happens when you add extreme partisanship to the mix?
It makes it untenable. Untenable! It makes people’s willingness to accept the dynamic nature of the science impossible.
We’re living in a progressively anti-science era and that’s a very dangerous thing when you’re dealing with a very deadly pandemic that has already killed more than a million people in this country.
Do you ever ask yourself where we would be now with HIV/AIDS if we had today’s level of partisanship back then?
I don’t think we would be as advanced as we are now.
Ideological differences are a good way of keeping balance in this country. But not when it turns into profound divisiveness.
An example is if you look at the number of people vaccinated in red states versus blue states. There is absolutely no reason whatever that you’d make a decision about whether or not you are going to avail yourself of a lifesaving intervention for yourself and your family based on your ideological persuasion. It just doesn’t make any sense.
You are among the most beloved doctors and scientists in the country and also among the most reviled. Are you OK with that?
For me personally, I don’t care. But I’m not OK with the country being so divisive that they threaten the life and the safety of people like me and my family merely because I’m telling people to get vaccinated, to wear a mask where appropriate, to avoid indoor settings, and to abide by public health principles.
I mean, if that’s the reason why I’m hated by people, that’s a sorry state for the country.
This interview has been edited for length and clarity.